盘点医疗器械国产替代热门领域,哪些行业已经蓄势待发?
2021-10-26
实现国产替代,在我国医疗器械领域一直是长久不衰的话题,同时也是众多细分领域一直以来的发展规划和目标。
近日,国家财政部及工信部联合发布的《政府采购进口产品审核指导标准》(2021年版)通知流出,该通知明确规定了政府机构(事业单位)采购国产医疗器械及仪器的比例要求。
其中137种医疗器械全部要求100%采购国产;12种医疗器械要求75%采购国产;24种医疗器械要求50%采购国产;5种医疗器械要求25%采购国产。采购范围覆盖监护仪、影像设备、体外诊断、高值耗材等多个品类。
近几年里,相关政策一直在为医疗器械的国产替代提供支持。一方面,部分政策以提高国产医疗企业创新能力为主要目标,并以提升医疗器械的审批质量、效率为重点,为实现国产替代打下基础。
另一方面,政策也在逐步加强对进口医疗器械的采购行为规范,我国多个省市均在其公布的政府采购政策中明确提出要严格限制进口医疗器械,以推进医疗机构中医疗设备的占有率。

今年以来部分有关国产医疗器械发展的政策
早在2007年,国家财政部就印发了关于《政府采购进口产品管理办法》的通知,主要是为了推动和促进自主创新政府采购政策的实施,以及规范政府在进口产品方面的采购行为。
今年以来,浙江省、广东省、四川省相继推出了最新的进口医疗设备采购清单,其中,广东省发布的采购清单中包含的进口器械数量更是呈现出了跳水式下降。
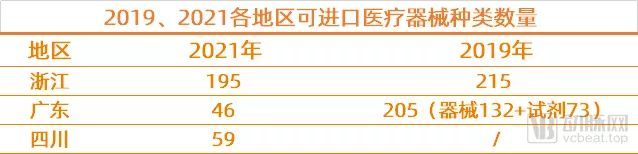

从中低端走向高端,国产替代的下一步
在政策的不断推动下,越来越多的优质国产器械走向市场,国产品牌的市场份额也不断扩大,过去主要依赖进口的基本医疗器械产品已基本实现国产化,国产替代也逐步从中低端市场走向高端市场。
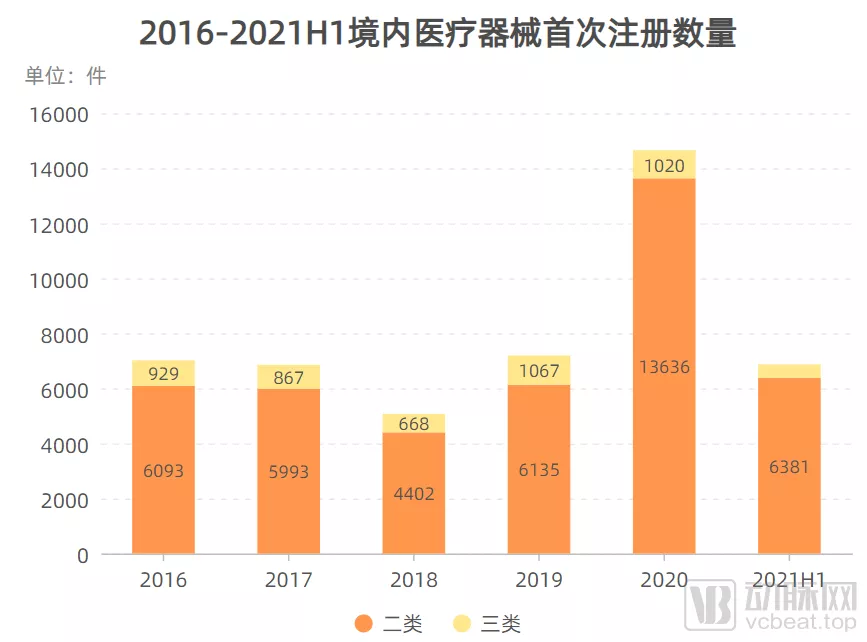
由上图可知,近年来国产获批二类、三类器械数量整体上处于上升状态,2020年受疫情影响,获批器械数量更是出现了爆发式增长。与之相反的是,近六年首次获批的进口医疗器械数量整体上呈逐年下降趋势。
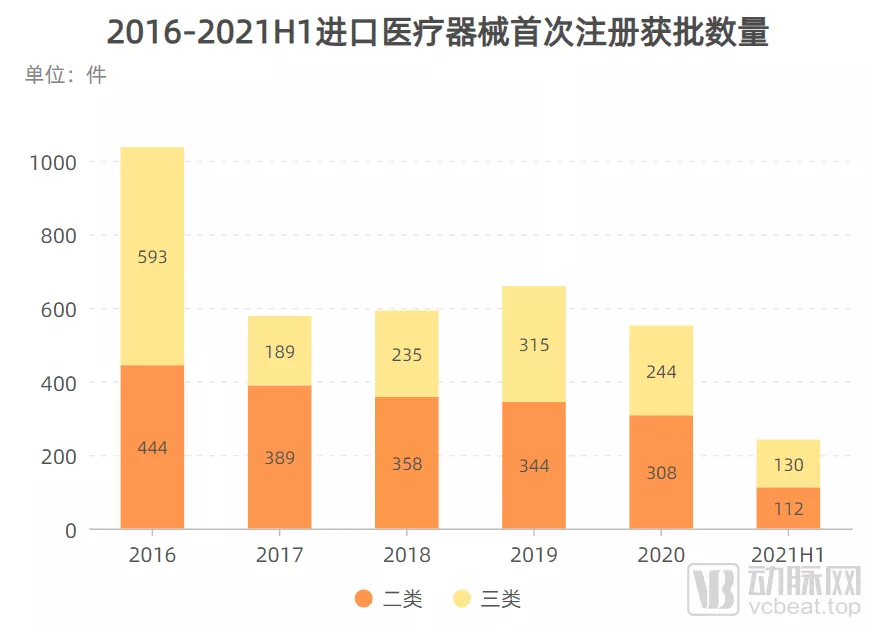
可以看出,境内二类器械获批数量远远大于进口二类获批数量,说明在中低端器械领域,国产基本实现替代,而境内三类获批器械数量不仅逐渐上升,且整体数量也已超越进口三类,这也在一定程度上意味着在高端医疗器械方面,国产替代开始加速。
获批产品类别方面,对比2018年和2020年全年境内三类器械的获批情况可以发现,在这两年时间里,口腔科器械、骨科手术器械、妇产科、辅助生殖和避孕器械、物理治疗器械、呼吸、麻醉和急救器械的获批数量增幅位列前五位,但同时这五类获批数量均处于较低水平。
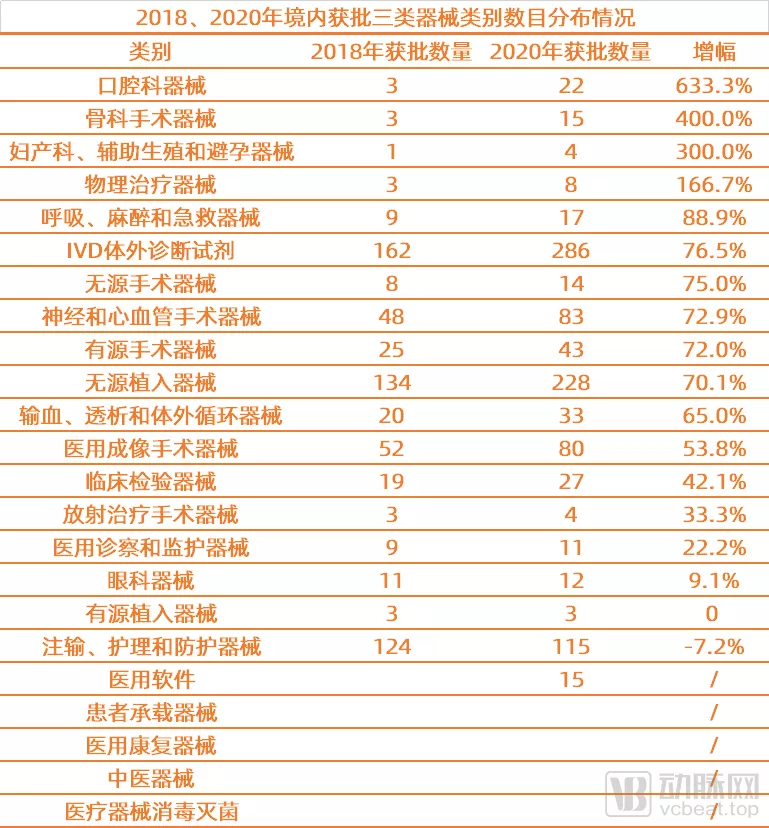
体外诊断试剂、无源植入器械、注输、护理和防护器械、神经和心血管手术器械、医用成像器械这五大类则一直位列获批前五位,这一情况在2021年上半年同样得到了延续(2021H1获批三类器械情况在后文再做分析)。
哪些领域实现了国产替代?
从获批数据上看,我国医疗器械大多细分领域的国产替代已经开始提速甚至于已实现国产替代,那么具体而言,我国哪些领域已经突破了技术壁垒,并基本实现了进口替代(国产占比超过50%)?
IVD-生化诊断
生化诊断是我国起步最早的体外诊断子行业之一,多年来一直是医院的常规诊断检测项目,目前我国生化诊断领域国产品牌的市占率已达到了70%,已经基本完成进口产品替代。 相对于IVD其他子领域而言,生化诊断试剂的技术壁垒较低。此外,上世纪末进口品牌进入中国时,由于生产成本及检疫、税收等原因,进口生化诊断试剂的价格普遍偏贵,因此生化诊断试剂成为了众多国产企业进入体外诊断领域和实现国产替代的切入点。
随着技术的不断完善和在生化诊断试剂上的经验积累,国内企业顺应行业发展趋势也开始发力生化仪器,并在技术和性能上追赶进口品牌,逐步实现生化诊断市场的国产替代。
现阶段,我国生化诊断领域整体上以国产品牌为主,但集中度较低,主要企业为迈瑞、科华生物、九强生物等。
监护仪
国产监护仪的发展过程,在某种程度上也对应着迈瑞的成长史。
90年代,我国监护仪市场为外企所垄断,而迈瑞通过早期代理进口产品的积累开始逐步走向自主研发的道路,并先后向市场推出了第一台国产血氧饱和监护仪和第一台国产多参数监护仪,打破了国外巨头的垄断。
随后,迈瑞不断加大研发投入力度,并且不断根据临床实际需要优化产品,监护仪也历经了“以单片机为核心-以PC为核心-以网络为核心”的转变。现阶段,迈瑞在监护仪领域已做到国际市场市占率第三,国内市场市占率第一(市占率超60%)。
冠脉支架
1998年,冠脉支架开始在我国广泛应用,此后的数年时间里,经皮冠状动脉介入(PCI)手术量及冠脉支架使用量均保持超高速增长。但我国对于心血管支架的研发较晚,早期国内相关市场基本上由强生、美敦力、波士顿科学等多家跨国巨头主导,这一情况在2004年得到了改变。
2004年,微创医疗上市了首个国产药物洗脱冠脉支架,随后乐普医疗和吉威医疗的新产品先后推出,凭借优良的技术性能和相对便宜的价格,国产冠脉支架开始迅速起量。据中国医疗器械行业外科植入物专业委员会统计数据显示,2006年、2007年、2008年国产支架市占率分别达到59%、65%、70%,国产冠脉支架“成功逆袭”,实现国产替代。
除上述领域外,DR、心脏封堵器等领域同样在国产替代方面取得了优异成绩。总结我国已经实现国产替代的器械细分领域的经验,可以看出,技术、性价比、品牌都是国产企业的制胜法宝。此外,在这一过程中,大多数企业选择在国内竞争格局尚未形成之前就推出产品,形成先发优势,快速抢占市场,从而跻身国产第一梯队。
国产替代,下一个锚点有哪些?
虽然近年来我国医疗器械市场发展势头不减,且已成为了全球第二大医疗器械市场,但不可否认的是,我国医疗器械领域中仍有多个细分领域是以进口为主导。
对此,动脉网通过分析2021年上半年获批三类器械的国产产品和进口产品数量以及进口产品的主要种类,试图分析不同领域的国产替代状态,寻找下一个在未来有望完成国产化的赛道。
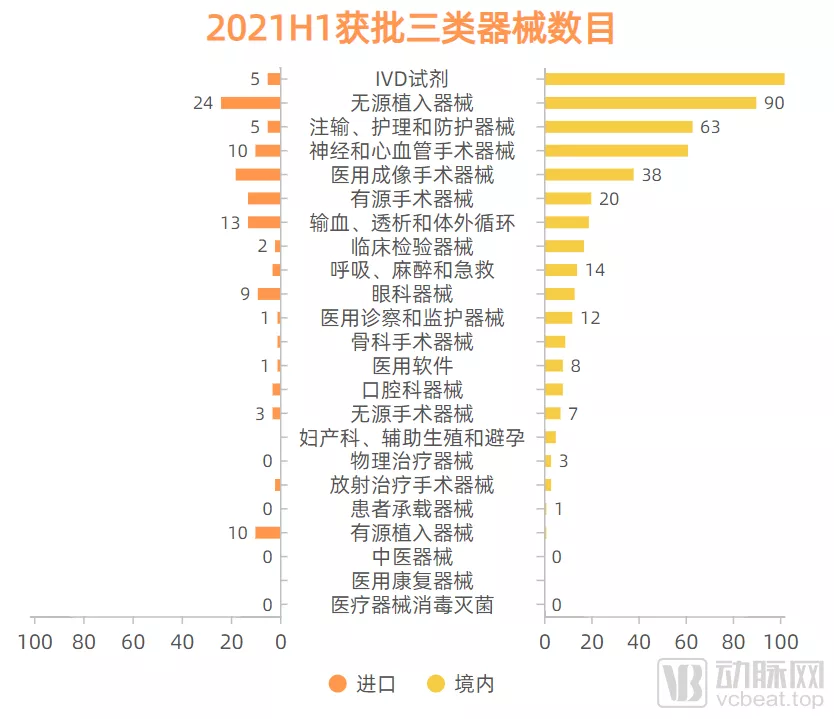
通过分析2021年上半年境内和进口获批三类器械的情况,可以看出有源植入器械、眼科器械、医用成像手术器械、有源手术器械等领域进口产品仍占有重要比例,在有源植入器械领域,进口产品更是远超国产产品。
一、有源植入器械:ICD植入式心律转复除颤器
在今年上半年获批的10个进口有源植入器械中,有约一半均是ICD。根据定义,ICD是一种植入患者胸腔内,通过除颤导线经静脉与心脏相连接,能自动识别并及时终止恶性室性心律失常的电子装置。
ICD同时具有除颤和起搏的功能,当患者心跳过速时,ICD能通过高能电脉冲转复为正常心律;而当患者心跳过缓时,ICD能通过低能电脉冲将心律恢复正常。合理使用ICD可以纠正快速性室性心律失常,减少猝死的发生率,延长患者寿命。多项临床证实,ICD是预防心脏性猝死的最佳治疗方法。
但在技术层面,ICD是将现代临床心脏电生理与起搏技术和现代微电子技术紧密结合的高科技成果,其产品系统集成复杂、对及时性、有效性和安全性有着极高的要求,又兼具起搏器提供的起搏功能,因此被公认是行业中技术门槛最高、研发风险最高的三类有源植入医疗器械之一。
虽然产品临床应用价值明显,但ICD在我国的普及率并不高,据国家卫生健康委员会心率失常介入质控中心上报数据,2018年中国大陆ICD植入量为4471例,远低于欧美国家的部分欧美国家的ICD植入量。
费用昂贵成ICD普及重要障碍
价格,是造成我国ICD设备普及不高的重要原因。现阶段临床常用ICD有两种,一般价格在6万到8万之间,部分产品价格高达10万-15万元,虽然部分费用可经医保报销,但对普通家庭而言依旧开销巨大。
且我国ICD领域尚未形成明确的治疗参考指南,市场教育存在不足,这些原因同样也是限制我国ICD植入量发展的重要因素。
此外,ICD在后期的应用和推广上也存在一些隐患。今年4月,美敦力就因为电池原因对ICD产品进行了主动召回,级别为一级。此前,波士顿科学、圣犹达(被雅培收购)等企业也都曾进行过ICD产品主动召回。作为植入体内的三类器械,ICD的安全性格外重要。
高壁垒的ICD领域,国内哪些企业在涉足?
市场方面,我国ICD领域呈进口垄断状态,暂无上市的国产ICD产品。
根据《2019-2023年中国植入性心律转复除颤器(ICD)市场分析可行性研究报告》显示,目前国内ICD市场主要被波士顿科学、美敦力、百多力、圣犹达等品牌占据。
进口垄断之下,部分国产品牌开始尝试布局这一研发难度高的领域,力争用原创产品抢占市场。
早在2014年,微创医疗便与索林(LivaNova旗下心律管理业务)成立了合资公司“创领心律管理”,共同研发、生产和营销心律管理器械(包括起搏器、ICD及CRT等)。
2015年,创领心律管理推出了PLATINIUMTM系列植入式除颤器,该产品具有全球最长的14.3年使用寿命,可降低频繁更换ICD可能产生的风险,海外市场反响良好。2018年,微创医疗宣布与云峰基金共同完成了对索林的收购,自此,微创医疗拥有了CRM(心脏节律管理)全套产品线。
另一家在ICD领域有所布局的企业则是来自苏州的无双医疗。自2017年成立以来,无双医疗就始终专注于CRM领域三类有源产品的研发和产业化,同时以ICD作为切入点。据了解,无双医疗的一代ICD产品已进入注册检验流程,并已申报创新医疗器械。
二、医用成像手术器械:内窥镜
医用成像手术器械领域实际上国产获批数量多于进口,但获批产品更多的集中在CT以及MRI方面。在今年上半年获批的18款进口三类医用成像手术器械中,内窥镜占据了重要比例。 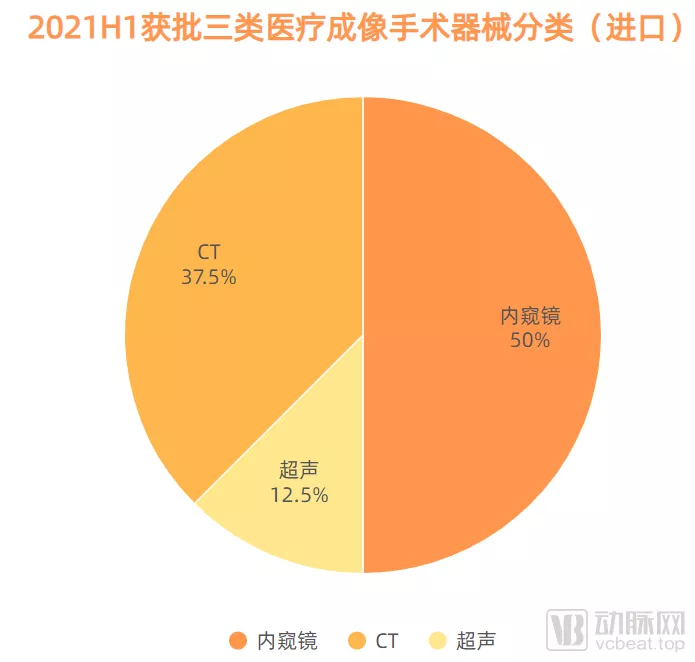
内窥镜自19世纪问世以来,不断发展,如今已应用于消化内科、呼吸科、普外科、耳鼻喉科、骨科、泌尿外科、妇科等科室,成为重要的医疗诊断和治疗设备。内窥镜发展至今,已有硬管式内窥镜、半可屈式内窥镜、纤维内窥镜和电子内窥镜四代产品。电子内窥镜由于更高的成像质量,已成为市场主流。
现阶段由于临床对微创治疗的需求增加,用于微创手术的内窥镜也再度迎来了发展良机。根据Evaluate MedTech公布的数据,2019年全球内窥镜市场销售规模达到209亿美元,未来五年将以6.3%的年均复合增长率持续增长,并于2024年达到283亿美元。
但我国内镜检查及微创治疗开展时间较晚,国内内窥镜企业的发展受到了一定的阻碍,目前国内内窥镜市场仍是以进口品牌为主导。《中国医疗器械行业发展报告2019》显示,卡尔史托斯、奥林巴斯、史赛克等海外巨头占据的内窥镜硬镜市场份额超90%,国产替代空间巨大。
逐步掌握核心技术,为内窥镜国产化带来机会
对于内窥镜这类技术壁垒高的设备而言,在核心部分和技术上实现突破显然是国产化的重中之重。
据了解,内窥镜的核心部件包含镜头、图像传感器、图像处理器、光源。目前,国内企业在图像处理器、光源等核心部件方面已实现突破,成为了内窥镜国产化的有力支撑。
图像传感器方面,随着CMOS图像传感器技术的崛起,原有的CCD图像传感器技术开始被替代。与CMOS相比,CDD制造难度大,核心技术被国外巨头限制,价格也更为高昂,而CMOS不仅技术壁垒相对较低,且耗能低,噪声小,其应用为内窥镜的国产化带来了机会。
随着技术的深入,内窥镜与众多创新技术、材料和工艺相互融合,并朝着小型化、多功能、图像高质量方向发展,随之衍生出了众多创新品类。现阶段,三维内窥镜、一次性内窥镜、胶囊内窥镜均是目前市场关注度较高的几类产品。
三维内窥镜:图像效果更直观
在成像方面,3D、4K与常规内窥镜相比更加直观和清晰,是目前大多数厂商的技术研发重点,其中三维内窥镜在一定程度上能够恢复自然视觉的优势,经图像处理器合成后的图像具有立体效果,使得观察到的画面解剖层次更明显,有利于提高手术效率。
就在今年,威高机器人的三维腹腔内窥镜成功获批,随后,速瑞医疗和微创医疗相继获得了三维电子腹腔内窥镜的NMPA批准,可见我国在三维内窥镜方面已取得初步成果。
一次性内窥镜:内窥镜耗材化,五家企业获批NMPA
传统内窥镜由于结构复杂,难以彻底清洗和消毒,这也导致了同一内窥镜在不同患者之间使用时存在的交叉感染风险。
一次性内窥镜作为解决这一问题的有效方案则应运而生。一次性内窥镜不仅在解决交叉感染问题上表现优异,而且一次性使用不存在对内窥镜的损耗,可以保证每次拆开包装内窥镜处于最佳状态,一定程度上提升了手术效率。
据不完全统计显示,目前国内一次性内窥镜领域已有5家企业获得NMPA注册证,产品获得了市场监管者的认可。
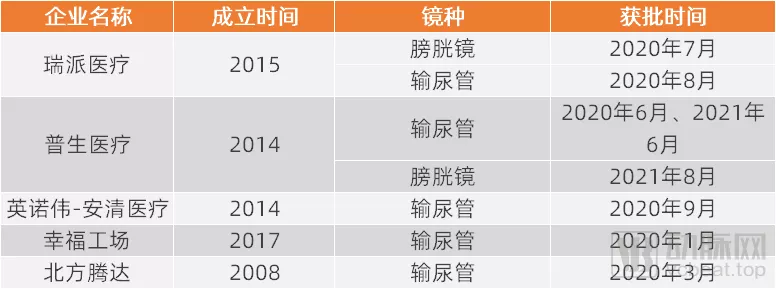
国内一次性内窥镜NMPA获批情况(部分)
胶囊内镜:操作便捷,解决传统胃肠镜检查痛点
一直以来,我国的消化道疾病发病率都居高不下,但是由于传统胃肠镜侵入式的检查方式给患者带来了较大的痛苦,患者积极性不高。而胶囊内镜则无需麻醉、舒适安全,且诊断准确率可以达到普通内镜效果,受到了更多患者的青睐。
此外,胶囊内镜在避免交叉感染方面同样也表现优异。据了解,安翰科技、金山科技、资福医疗、尚贤医疗均已推出胶囊内镜产品,并销往全球各地。
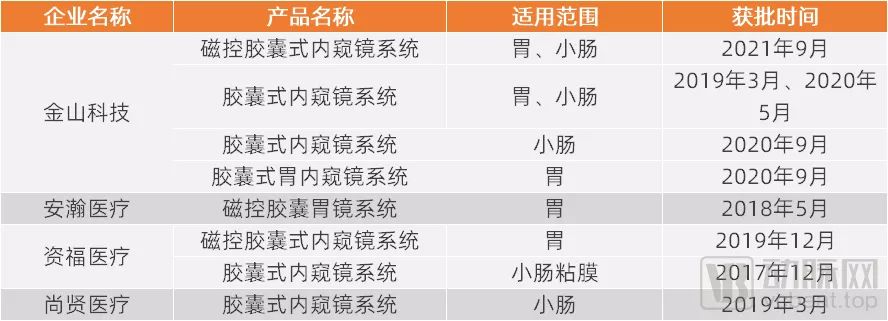
国内胶囊内镜NMPA获批情况(部分)
除上述类别外,超声内镜这一将内镜和超声相结合的消化道检查技术同样也是内窥镜的一个创新方向。现阶段在超声内镜领域奥林巴斯、富士和宾得已有产品上市,国内开立医疗在这一领域已经有所布局,但整体上国内并未有国产超声内镜上市,同样存在巨大的国产替代空间。
三、无源植入器械:神经内/外科植入物
在今年上半年获批的进口无源植入器械中,神经内/外科植入物、关节置换植入物、骨科填充和修复材料等产品为主要进口类别,其中神经内/外科植入物所涉及的神经介入市场正是我国亟需国产替代的领域之一。
据归创通桥招股说明书显示,现阶段我国神经介入市场被美敦力、强生、史赛克等外资企业占据93%的市场,而国产企业正从无到有构建完整产品线。
神经介入市场主要包含针对缺血性中风和动脉狭窄的缺血类产品、针对动脉瘤的出血类产品及辅助建立通路的通路类产品。其中,缺血类产品由于患者更多,市场空间更大;出血类产品由于疾病复杂,操作难度更大,技术壁垒更高;通路类产品由于技术壁垒较低,已实现部分国产化。
在资本方面,神经介入颇得投资者青睐。据动脉网不完全统计,今年以来,神经介入领域已有8起融资并购事件,可以说相比已经成功实现国产替代的冠脉介入领域,神经介入所面临的资本环境更加友好。
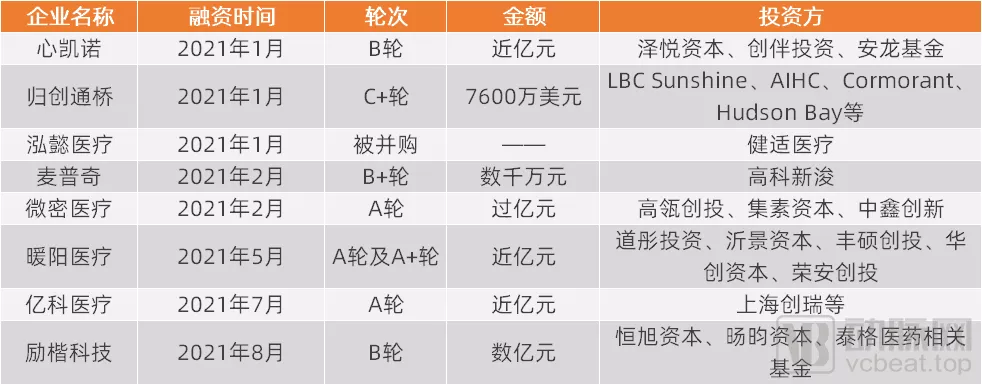
在产品质量方面,国产神经介入产品在质量上进步明显,甚至有些产品的部分指标优于进口产品,不过球囊、覆膜支架、密网支架、动脉支架等产品国产的上市数量较少,相关市场有待进一步攻破。
造成国产神经介入产品渗透率低的原因是多方面的,产品价格、患者认知、脑血管疾病筛查、卒中中心数量等因素都对其造成了一定影响,这也是未来神经介入领域器械需要突破的地方。
来源:动脉网











