中国科大吴东、胡衍雷:研制远程可控的磁控微纳机器人用于靶向药物治疗
2020-01-06
诺贝尔奖得主理论物理学家理查德·费曼曾在1959年率先提出利用微型机器人治病的想法,用他的话说,就是将“外科医生”吞下。随着微纳米加工技术的发展,加工这些可以被吞下的“外科医生”成为现实,人们通常把这些“外科医生”称为人造微纳机器人。受自然界微生物自由运动启发,人造微纳机器人近些年得到了广泛的关注与研究,通过电场、磁场、光场等手段可以有效地驱动这些微纳机器人,在无创手术、靶向药物运输和生物传感检测等领域具有广泛的应用。在多种驱动方案中,磁场驱动可以无线式精确操纵微纳机器人,改变外部磁场梯度和方向,会对微纳机器人施加力和力矩,进而使其沿着期望的轨迹运动。
近期,中国科学技术大学工程科学学院微纳米工程实验室在利用调制结构光场高效加工微纳机器人及其细胞移植、靶向药物运输方面取得重要进展。他们通过将调制的涡旋光束进行单次快速曝光或三维空间扫描加工出泳动性能与装载货物能力更强的空心管形和锥形螺旋结构,并利用该结构进行神经干细胞的体外移植、靶向药物运输治疗肿瘤细胞。相关成果分别以“Conical Hollow Microhelices with Superior Swimming Capabilities for Targeted Cargo Delivery”和“Targeted Single-Cell Therapeutics with Magnetic Tubular Micromotor by One-Step Exposure of Structured Femtosecond Optical Vortices”为题发表在Advanced Materials和Advanced Functional Materials [Adv. Mater., 31, 1808226, 2019; Adv. Funct. Mater., 29, 1905745, 2019]。
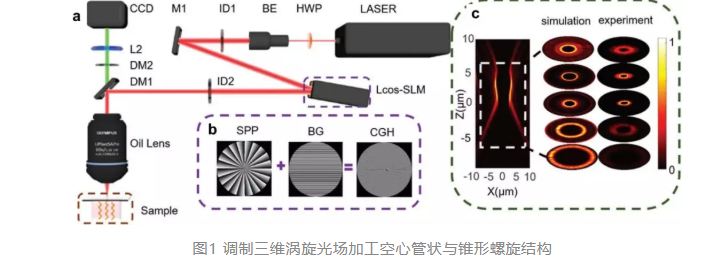
在上述工作中,研究人员设计具有特殊相位信息的光场全息图,并将其加载于空间光调制器面板上,调制出的三维涡旋光场可用于高效加工空心管状和锥形螺旋结构,相比于传统的激光直写加工(DLW),光场加工速度最快提高了600倍。除此之外,利用该方法也可以灵活可控地加工出不同参数的管状与螺旋结构,大大提高了复杂三维结构的加工能力。
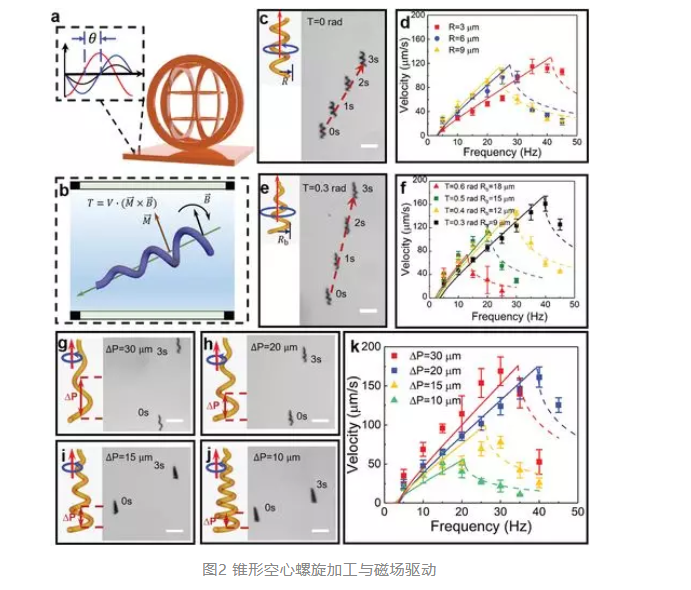
其次,利用如图2所示的锥形空心螺旋结构,并在其表面加入磁性响应材料。采用自行搭建的三维亥姆霍兹线圈控制系统,调节输入电流的相位信息在三维空间内形成旋转磁场,磁场方向的改变使磁性结构受到磁力矩作用,进而完成有效驱动。经对比发现锥形螺旋相比于传统的直螺旋结构具有更快的前进速度,并有效抑制了横向漂移运动。
除此之外,利用磁场梯度和方向的变化可以有效完成微结构的精确导向,空心锥形螺旋在旋转磁场下完成各种复杂图案化轨迹运动(如图3所示),空心管状结构在梯度磁场下完成SiO2微球的装载、运输、排列与释放。
最后,研究人员利用锥形空心螺旋结构内部与外部分别装载纳米及微米级货物,并在体外完成了神经干细胞的移植;利用管装微结构装载运输抗癌药物(DOX)对癌细胞(Hela)进行有效治疗,并通过荧光验证治疗效果。这些工作提出了简单稳定的空心管状、锥形螺旋微电机加工操纵技术,在细胞移植、体内药物运输、无创手术等领域具有重要应用前景,为相关生物医疗领域提供了新的技术手段。
工程科学学院博士生辛晨、杨亮为论文的第一作者,吴东教授和胡衍雷副教授为论文的共同通讯作者。这项工作得到了国家自然科学基金重大仪器、中国科学院和科技部重点研发计划的支持。
来源:中国科技大学
声明:仅代表作者个人观点,作者水平有限,如有不科学之处,请在下方留言指正!











